What is the Kyphoplasty?
Kyphoplasty is a pivotal procedure in the realm of pain management for patients suffering from vertebral compression fractures (VCFs), primarily those caused by osteoporosis, malignancy, or trauma. This minimally invasive surgical technique aims not only to alleviate the severe pain associated with these fractures but also to stabilize the affected vertebra and restore its height, potentially reversing some of the deformity and improving the patient's posture and overall spinal alignment. By directly addressing the structural cause of pain, kyphoplasty offers a significant and immediate reduction in pain levels for many patients, allowing them to return more quickly to their daily activities and significantly improving their quality of life.
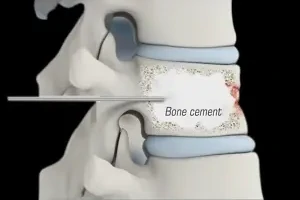
The procedure involves the percutaneous insertion of a balloon into the collapsed vertebra, which is then inflated to lift the bone fragments and return them to a more normal position. Following balloon deflation, the created space is filled with bone cement to secure the vertebra's structure. The benefits of kyphoplasty from a pain management perspective include a rapid decrease in back pain, increased mobility, and decreased use of pain medication post-procedure. Furthermore, by restoring vertebral height and reducing spinal deformity, kyphoplasty can help prevent the long-term complications associated with vertebral compression fractures, such as chronic pain and impaired pulmonary function. With its minimally invasive nature, kyphoplasty presents a lower risk profile compared to traditional open surgery, making it a valuable option for patients seeking effective pain relief and structural spinal recovery.
What are the benefits and risks of the Kyphoplasty?
Kyphoplasty offers a minimally invasive solution for patients suffering from vertebral compression fractures, presenting both benefits and risks.
Benefits
- Pain Relief: Kyphoplasty often provides immediate and significant reduction in back pain associated with vertebral compression fractures.
- Restoration of Vertebral Height: The procedure can partially or fully restore the height of the collapsed vertebra, improving posture and spinal alignment.
- Stabilization of Fracture: By injecting bone cement into the vertebral body, kyphoplasty stabilizes the fracture, which reduces pain and prevents further collapse.
- Improved Mobility: Patients typically experience improved mobility and are able to return to their daily activities more quickly after the procedure.
- Minimally Invasive: Compared to open spine surgery, kyphoplasty is less invasive, involves smaller incisions, less muscle damage, and typically results in shorter hospital stays and recovery times.
- Decreased Use of Pain Medication: Effective pain relief from kyphoplasty can reduce the need for pain medication, decreasing the risk of side effects associated with long-term use.
Risks
- Infection: As with any surgical procedure, there is a risk of infection at the incision site or within the vertebral body.
- Bleeding: There is a small risk of bleeding during the procedure.
- Nerve Damage: Though rare, there is a possibility of nerve damage resulting in numbness, tingling, or weakness.
- Cement Leakage: One of the specific risks of kyphoplasty is the leakage of bone cement into surrounding areas, which can potentially compress spinal nerves or enter the bloodstream.
- Allergic Reaction: There is a risk of allergic reaction to the materials used, such as the bone cement or anesthesia.
- No Improvement or Worsening of Pain: In some cases, patients may not experience significant pain relief, or their pain may worsen after the procedure.
- New Fractures: There is a possibility of developing new vertebral fractures, particularly in vertebrae adjacent to the treated area, due to changes in spinal biomechanics or continued bone weakening.
Kyphoplasty is a valuable procedure for many patients suffering from vertebral compression fractures, offering significant benefits in pain management and mobility. However, it is important to discuss the potential risks and benefits during a consultation to make an informed decision based on your specific health condition and treatment goals.
Who is a good candidate for the Kyphoplasty?
Good candidates for kyphoplasty are typically individuals experiencing painful vertebral compression fractures (VCFs), especially those fractures that have not responded to conservative treatment methods. Key characteristics of suitable candidates include:
- Osteoporosis-Related Fractures: Individuals with osteoporosis who have suffered vertebral compression fractures are prime candidates, as kyphoplasty can provide both pain relief and vertebral stabilization.
- Cancer-Related Fractures: Patients with fractures due to cancer or cancer treatments (like radiation) affecting the vertebrae may benefit from the procedure to alleviate pain and restore vertebral height.
- Acute Pain from Recent Fractures: The procedure is most effective for treating recent fractures, generally within a few months of occurrence, before the bone has fully healed. Patients with acute pain from recent fractures that significantly impacts their quality of life and mobility are ideal candidates.
- Inadequate Relief from Conservative Treatments: Those who have not experienced sufficient pain relief from non-surgical treatments, such as pain medication, physical therapy, or bracing, may find kyphoplasty to be a beneficial option.
- Ability to Tolerate the Procedure: Good candidates should be in adequate overall health to undergo the procedure, considering factors like anesthesia and the potential risks of surgery.
- Intact Posterior Vertebral Wall: Ideal candidates should have fractures where the posterior vertebral wall is largely intact to minimize the risk of cement leakage during the procedure.
Kyphoplasty may not be suitable for all patients, such as those with vertebral fractures due to certain infections, those with bleeding disorders, or those who have fractures that have already healed. During a thorough evaluation, including imaging studies and a comprehensive medical history, we can determine if kyphoplasty is the right treatment option for you.
How is a Kyphoplasty performed?
Here’s an overview of how kyphoplasty is typically performed:
- Preparation and Anesthesia: The patient is positioned prone (lying face down) on the operating table. Local anesthesia with sedation or general anesthesia is administered to ensure the patient is comfortable and pain-free during the procedure.
- Fluoroscopic Guidance: A fluoroscope, a type of X-ray machine, provides real-time imaging to guide the surgeon in placing the instruments accurately within the vertebral body.
- Access to the Vertebra: A small incision is made in the back, through which a hollow needle (trocar) is inserted and carefully guided into the fractured vertebra.
- Balloon Inflation: Once the needle is in the correct position, a small, balloon-like device is inserted through the needle into the vertebral body. The balloon is then gradually inflated, which helps to elevate the fracture, restoring some of the lost vertebral height and creating a cavity within the vertebra.
- Cement Injection: After the balloon is deflated and removed, the created cavity is filled with a special bone cement (polymethylmethacrylate or PMMA). The cement quickly hardens, stabilizing the fracture and preventing further collapse of the vertebra.
- Closure: The instruments are removed, and the small incision is closed using sutures or adhesive strips. The procedure typically takes about an hour per vertebra treated.
- Recovery: Patients are usually monitored for a short period before being discharged, often on the same day. Recovery involves following specific instructions from the healthcare team, including any restrictions on activity and follow-up appointments.
Kyphoplasty can offer significant pain relief and improved mobility for patients with vertebral compression fractures. However, it's important for patients to discuss the potential benefits and risks of the procedure to determine if it's the right option for them.