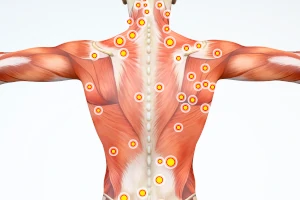
What are Trigger Point Injections?
Trigger Point Injections (TPI) are a pain management treatment aimed at alleviating discomfort in muscles that contain trigger points, or tense knots of muscle that fail to relax and can cause widespread pain. These trigger points may also refer pain to different areas of the body when pressed. During a TPI procedure, a healthcare provider inserts a small needle into the trigger point and injects a solution, typically containing a local anesthetic and sometimes a corticosteroid, to deactivate the trigger point and alleviate pain. This method can effectively treat conditions such as myofascial pain syndrome, fibromyalgia, tension headaches, and chronic muscle pain that does not respond to other treatments.
The procedure is quick, usually performed in a doctor's office, and patients can often return to their normal activities shortly afterward. TPI can provide immediate relief from muscular pain and improve flexibility and range of motion. While some patients may experience significant improvement after just one treatment, others with chronic conditions might require multiple injections over time to maintain pain relief. TPIs are considered a safe and effective way to manage specific types of pain, especially when used as part of a comprehensive pain management plan.
What are the benefits and risks of Trigger Point Injections?
Trigger Point Injections (TPI) offer several benefits for individuals suffering from muscle pain and discomfort, but like any medical procedure, they also carry certain risks.
Benefits
- Immediate Pain Relief: Many patients experience rapid relief from pain and discomfort following a TPI, as the injection helps to relax the muscle knot and alleviate tension.
- Improved Mobility: By deactivating trigger points, TPIs can enhance range of motion and flexibility, making it easier for patients to engage in physical therapy and daily activities.
- Minimal Invasiveness: TPIs are a minimally invasive treatment option that can be a preferable alternative to surgery for managing muscle pain.
- Low Downtime: The procedure is quick, and patients can often return to their normal activities shortly afterward with minimal recovery time.
- Diagnostic Tool: TPIs can also serve a diagnostic function by helping to identify the specific muscles contributing to pain.
Risks
- Injection Site Reactions: Patients may experience pain, bruising, or bleeding at the injection site. Infection is rare but possible.
- Temporary Numbness or Weakness: The local anesthetic used in the injection can cause temporary numbness or weakness in the treated muscle.
- Allergic Reactions: Though uncommon, some patients may have an allergic reaction to the medication used in the injection.
- No Relief from Symptoms: In some cases, TPIs may not provide the expected relief from muscle pain, necessitating alternative treatments.
- Reoccurrence of Trigger Points: TPIs treat the symptom of trigger points but may not address the underlying cause, leading to potential reoccurrence.
Discuss the potential benefits and risks of Trigger Point Injections with us during a pain management consultation to determine if this treatment is appropriate for your specific condition and overall health profile.
Who is a good candidate for Trigger Point Injections?
Good candidates for Trigger Point Injections (TPI) are individuals experiencing myofascial pain syndrome, chronic muscle pain, or discomfort associated with trigger points—localized, tender knots in the muscle that can cause pain in the muscle and sometimes in seemingly unrelated parts of the body (referred pain). Ideal candidates typically share the following characteristics:
- Chronic Muscle Pain: Those who have persistent muscle pain that has not responded to conventional treatments such as physical therapy, massage, or oral pain relievers.
- Identifiable Trigger Points: Individuals with palpable trigger points that cause pain or discomfort, either locally or through referred pain, and that can be precisely targeted with an injection.
- Functional Limitation: Patients whose pain limits their mobility or daily activities, affecting their quality of life.
- No Relief from Other Modalities: Those who have tried other pain management techniques (e.g., heat therapy, physical therapy, or oral medications) without sufficient relief.
- Seeking Minimally Invasive Options: Patients interested in minimally invasive procedures as an alternative to more aggressive treatments or surgery.
- Absence of Contraindications: Individuals without skin infections, bleeding disorders, or allergies to the injectable substances used in TPIs.
Candidates should undergo a thorough evaluation by a healthcare provider, who can assess their pain, identify trigger points, and review their medical history to ensure that TPI is an appropriate treatment option. This evaluation often includes a physical examination and, in some cases, diagnostic imaging to rule out other causes of pain.
How is a Trigger Point Injection performed?
A Trigger Point Injection (TPI) is a straightforward procedure designed to treat painful areas of muscle that contain trigger points, or knots of muscle that form when muscles do not relax. Here's how the procedure is typically performed:
Preparation
- Assessment: The healthcare provider first identifies the specific trigger points by palpating (examining by touch) the muscle. These areas are often tender and may produce a twitch response when pressed.
- Informed Consent: Before proceeding, the patient is informed about the benefits, risks, and any alternatives to the procedure, and consent is obtained.
The Procedure
- Positioning: The patient is positioned comfortably, usually sitting or lying down, to allow easy access to the affected muscle.
- Sterilization: The skin over the trigger point is cleaned with an antiseptic solution to reduce the risk of infection.
- Anesthesia: While not always necessary, a local anesthetic may be applied to the skin to minimize discomfort during the injection.
- Injection: A small needle is inserted directly into the trigger point. The injection contains a solution, typically consisting of a local anesthetic and, in some cases, a corticosteroid to reduce inflammation. For some conditions, dry needling (insertion of a needle without injecting any substance) may also be performed.
- Medication Delivery: Once the needle is correctly positioned in the trigger point, the medication is injected. This may cause a brief period of discomfort or a muscle twitch, known as a "jump sign," indicating that the trigger point has been accurately targeted.
- Withdrawal and Dressing: After the injection, the needle is withdrawn, and a small bandage is applied to the injection site.
Post-Procedure
- Observation: Patients are typically observed for a short period after the injection for any adverse reactions.
- Instructions: Patients are given post-procedure care instructions, which may include applying ice to the area to reduce soreness and instructions on activity levels.
- Recovery: Most patients can resume their normal activities shortly after the procedure, though some may experience temporary soreness at the injection site.
TPIs are generally considered safe and effective for managing muscle pain associated with trigger points. They can provide significant relief, improve muscle function, and can be repeated if necessary, depending on the patient's response to the treatment.