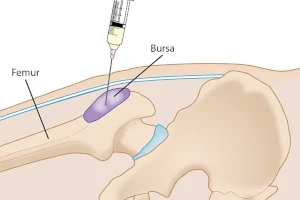
What is a Bursa Injection?
A bursa injection is a medical procedure used to reduce inflammation and pain in a bursa, a small, fluid-filled sac that acts as a cushion between bones and soft tissues, such as muscles, tendons, and skin, in various parts of the body. Bursae help reduce friction and allow free movement of joints and muscles. When a bursa becomes inflamed, a condition known as bursitis, it can cause significant pain and restrict movement.
The procedure involves injecting medication directly into the affected bursa. This medication typically includes a corticosteroid to quickly reduce inflammation and pain, and may also include a local anesthetic to provide immediate pain relief. Bursa injections are commonly performed in areas where bursitis is most prevalent, such as the shoulder (subacromial bursa), hip (trochanteric bursa), knee (prepatellar bursa), and elbow (olecranon bursa). The injection is usually done under sterile conditions and may be guided by ultrasound to ensure accurate placement of the needle. Bursa injections offer rapid relief from pain and inflammation and can be an effective part of a comprehensive treatment plan for bursitis, allowing patients to return to normal activities with improved comfort and mobility.
What are the benefits and risks of a Bursa Injection?
Bursa injections, typically involving the administration of corticosteroids directly into the bursa (a fluid-filled sac that reduces friction between tissues of the body), offer a targeted approach to reducing inflammation and pain in joints affected by bursitis or other inflammatory conditions. These injections can provide significant benefits but also come with potential risks.
Benefits
- Rapid Pain Relief: Bursa injections can quickly reduce pain and discomfort, often providing relief within a few days of the procedure.
- Reduced Inflammation: The corticosteroids used in the injections are potent anti-inflammatory agents, effectively reducing swelling and inflammation in the affected bursa.
- Improved Mobility: By alleviating pain and inflammation, these injections can enhance joint mobility, making daily activities and physical therapy more manageable.
- Minimally Invasive: The procedure is less invasive compared to surgery, with no significant downtime, allowing patients to return to their normal activities shortly after.
- Diagnostic Utility: In some cases, bursa injections also help in diagnosing the source of pain by confirming the bursa's involvement in the joint discomfort.
Risks
- Infection: Though rare, there is a risk of infection at the injection site or within the bursa.
- Allergic Reactions: Some individuals may experience allergic reactions to the medication used in the injection.
- Bleeding: There is a small risk of bleeding within the bursa following the injection.
- Post-injection Flare: A temporary increase in pain, known as a post-injection flare, can occur in the days following the procedure.
- Tendon Rupture: Repeated injections into or near tendons can weaken the tendon structure, potentially leading to rupture.
- Skin Discoloration: The skin over the injection site may lighten, especially in people with darker skin tones.
- Elevated Blood Sugar Levels: Patients with diabetes might experience a temporary spike in blood sugar levels after receiving a corticosteroid injection.
If you are considering bursa injections, discuss the potential benefits and risks with us during a pain management consultation. We will help you determine if this treatment is appropriate for your specific condition and overall health profile.
Who is a good candidate for a Bursa Injection?
Good candidates for Trigger Point Injections (TPI) are individuals experiencing myofascial pain syndrome, chronic muscle pain, or discomfort associated with trigger points—localized, tender knots in the muscle that can cause pain in the muscle and sometimes in seemingly unrelated parts of the body (referred pain). Ideal candidates typically share the following characteristics:
- Diagnosed with Bursitis: Patients with a clear diagnosis of bursitis confirmed through clinical examination and possibly imaging studies like ultrasound or MRI, indicating inflammation of one or more bursae.
- Localized Pain and Inflammation: Those who have localized pain and swelling in joints such as the shoulder (subacromial bursitis), hip (trochanteric bursitis), elbow (olecranon bursitis), or knee (prepatellar bursitis) that significantly impacts their daily activities and quality of life.
- Failed Conservative Management: Individuals who have tried and not responded to non-invasive treatments, including physical therapy, NSAIDs, and activity modification.
- Need for Rapid Relief: Patients seeking quick relief from pain and inflammation to return to normal activities or to participate more effectively in a rehabilitation program.
- No Contraindications: Those without skin infections, bleeding disorders, or allergies to the injectable medication proposed for use in the bursa injection.
We can provide a thorough evaluation to ensure that a bursa injection is the most suitable treatment option for you based on your specific situation and overall health.
How is a Bursa Injection performed?
Here's a step-by-step overview of how a Bursa injection is typically performed:
Preparation
- Patient Evaluation: The healthcare provider conducts a thorough assessment, including a review of the patient’s medical history and a physical examination, to confirm that bursitis is the source of pain. Imaging studies, such as ultrasound or MRI, may also be used to guide the injection.
- Informed Consent: The patient is informed about the procedure, including its benefits, risks, and any alternatives. Informed consent is obtained prior to proceeding.
The Procedure
- Positioning: The patient is positioned to comfortably access the affected bursa. The area around the injection site is cleaned with an antiseptic solution to minimize the risk of infection.
- Local Anesthesia: A local anesthetic may be applied to numb the skin and underlying area around the bursa to reduce discomfort during the procedure.
- Guidance: Ultrasound or fluoroscopy (a type of real-time X-ray) is often used to precisely locate the affected bursa and guide the needle to the correct spot. This imaging ensures accurate placement of the injection and enhances the safety and effectiveness of the procedure.
- Injection: Once the needle is correctly positioned, a mixture containing a corticosteroid (to reduce inflammation) and possibly a local anesthetic (to provide immediate pain relief) is injected into the bursa.
- Withdrawal and Dressing: After the medication is injected, the needle is withdrawn, and a small bandage is applied to the injection site.
Post-Procedure
- Observation: The patient is monitored for a short period after the injection for any adverse reactions.
- Instructions: Patients are usually advised to rest the affected joint and apply ice to reduce any soreness at the injection site. Specific instructions regarding activities and follow-up care are provided.
- Follow-Up: A follow-up appointment may be scheduled to assess the effectiveness of the injection and determine the need for further treatment.
Bursa Injections can provide significant relief from pain and inflammation associated with bursitis, improving joint function and patient mobility. The procedure is quick, and most patients can resume their normal activities shortly afterward, with some experiencing immediate pain relief.